Welcome to Focus On The Fight, a series of interviews that will be posted weekly, focusing on a blogger/advocate, their health and their advocacy work.
This week we meet Collin Wong, and we will highlight: Inflammatory Bowel Disease, aka Crohn’s.
Before we jump into the full interview, Collin, please tell us a little about you outside of your health! Tell us about your hobbies or family!
I am a soon-to-be freshman at Case Western Reserve University, with a focus on pre-med. In fact, I hope to be a pediatric critical care physician one day! In my free time, I enjoy doing graphic design and playing the piano.
What Chronic Illness (es) have you been diagnosed with? Which one will you focus on today?
I have Crohn’s Disease, which is a type of Inflammatory Bowel Disease (IBD).
Before we get into Collin’s interview, let’s take just a second to look at Inflammatory Bowel Disease.
What is Inflammatory Bowel Disease (IBD)?
Inflammatory Bowel Disease (IBD) is an umbrella term that is used to encompass Crohn’s disease, and Ulcerative Colitis, which are both characterized by inflammation of the gastrointestinal tract. That being said Crohn’s and Ulcerative Colitis are quite different. Let’s take a moment to look at characteristics of both conditions and what part of The gastrointestinal (GI) tract they impact. Please note that IBD IS NOT THE SAME AS IBS
-
Crohn’s- Can affect any part of the GI tract (from the mouth to the anus)— But in most cases it affects the portion of the small intestine before the large intestine/colon. Upon visual inspection the areas damaged appear in patches that are next to areas of healthy tissue. And the inflammation may reach through the multiple layers of the walls of the GI tract
-
Ulcerative Colitis (UC)- UC is most often found in the large intestine (colon) and the rectum. Upon visual inspection areas damaged by UC are continuous (not patchy) – usually starting at the rectum and spreading further into the colon. And inflammation is present only in the innermost layer of the lining of the colon
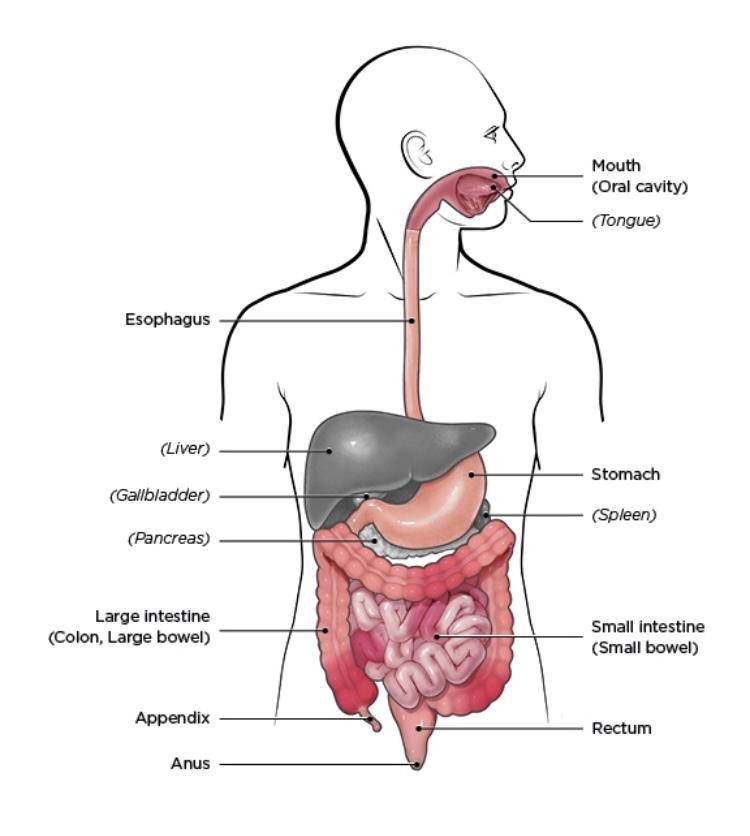
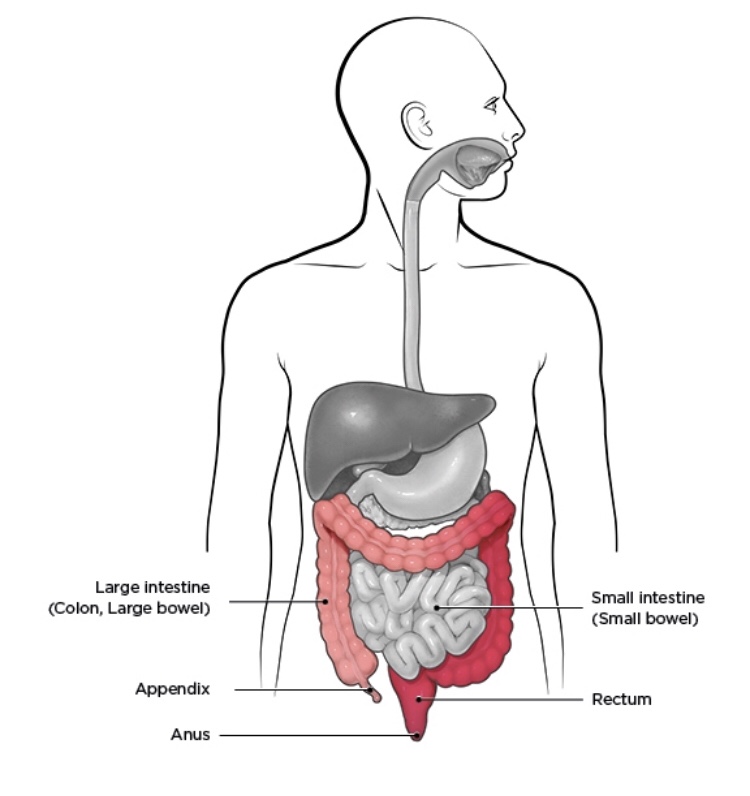
What are the symptoms of IBD?
-
Abdominal pain
-
Persistent Diarrhea
-
Rectal bleeding/bloody stools
-
Weight loss
-
Fatigue.
What causes IBD?
Sadly, like so many autoimmune conditions the cause of IBD is unknown at this time. Research has shown that it is in fact an autoimmune condition and is a result of a defective immune system. In a person with a healthy, and a properly functioning immune system, the immune system attacks foreign organisms, like viruses or bacteria to protect the body. But for those with IBD the immune system responds incorrectly to environmental triggers and attacks the body rather than the foreign organisms, causing inflammation of the gastrointestinal tract. Research has also found that there is a genetic component to IBD. Meaning if there is someone in your family with IBD, the likelihood of you developing IBD increases.
How is IBD diagnosed?
IBD can be diagnosed a couple different ways. When a patient first starts complaining of GI issues the dr will most likely order blood work &/or a stool sample which can show if the pain/symptoms are being caused by an infection or something else. From there they can order MRI’s or CT scans with contract to get a look at what’s going on with the bowel. A final diagnosis usually requires images from the diagnostic studies as well as results from either an endoscopy (for Crohn’s), or a colonoscopy (for UC).
How is IBD Treated?
There are several different options as far as medication goes for treatment of IBD, there are aminosalicylates, corticosteroids (i.e. prednisone), immunomodulators, and the newly approved biologics. Not all cases will respond to medication, and some severe cases may require surgery, those cases may require removal of the damaged portions of the GI tract. That being said with the new advances in medication the cases requiring surgery are becoming less common.
Now let’s jump into the interview.
Collin, please share briefly what led you to the decision to become a blogger (and patient advocate if applicable)who focuses on chronic illness.
I always wanted to be a blogger or YouTuber, but I put that aspiration away after freshman year of high school. I simply had no time to do any of that. One day during my internship last summer, I was having an especially slow day. It was July 3rd, and my mentor was on vacation for the weekend. After lunch, I started writing a college essay about my Crohn’s Disease, and I really enjoyed writing about it! The ideas just flowed naturally from my fingertips to the keyboard, and I could not stop thinking about it. I was officially obsessed. I realized that this had to be the time. All the ideas were fresh in my mind, and I had a lot of time during my internship. Was it impulsive? Yes. Worth it? Yes.
Diagnosing a Chronic Illness can sadly be a VERY long process! For you, how long did it take for an official diagnosis? Did you have to act your own advocate to get a doctor to take what was going on in your life seriously and look for a diagnosis?
I was not able to be my own advocate because I was only six at the time. Instead, my parents spoke for me. Thankfully, my doctor took my parents’ concerns seriously, and he promptly started evaluating. It took about a month to finish running all blood tests and imaging.
Chronic illness is just that, chronic. Please share with us how your illness (s) impacts your daily life!
Morning routines took a lot longer. From taking out the nasogastric tube to cleaning it, I spent a good part of my routine standing at the sink. IBD sometimes negatively affects my self-esteem too.
Being that you are so young, have you found that your illness has had a negative impact on your teenage years?? In the sense of issues with friends, or dating, or what colleges you looked at!?
My disease limited which colleges I applied to. I wanted to be close enough to home that if there was a medical emergency, my parents could still visit me in the hospital. Although, dating and friendships have not been a problem.
Sadly, being chronically ill can take a toll on all kinds of relationships. Have you noticed this in your life? If so how has your health impacted the relationships in your life?
I was more stressed out, so I was more easily frustrated with my parents. It was really hard for all of us to cope with my diagnosis.
Living with chronic illness can be life changing. Have you found that your life has changed significantly over the years of living with your condition? If so, in what ways has it changed?
My disease has changed me mostly positively. My disease has made me aspire to become a doctor. This happened during my shadowing experience because I was shadowing an IBD physician. I guess you can say that I was forced to confront my disease (before that, I had no plans on becoming a doctor). After that experience, I was set on becoming a doctor and a disease advocate for life. So it really was a combination of my disease and my shadowing that changed me.
All diseases have different kinds of flare ups, and every one will exhibit different signs of flare ups. For you what signs do you know to watch when a flare is coming your way?
I mostly vomit and sometimes have diarrhea.
What do you do to treat your flares? Or to make your bad days better?
I use lots of heat pads and take a mental health day.
Being diagnosed with a chronic illness can be very overwhelming. If you could give one piece of advice to someone who is going through the diagnosis process, or is newly diagnosed, what would it be?
Always pay attention to mental health … looking for red flags of depression is crucial.
Living with a chronic condition is hard, it just is! Especially because for the most part there are no outward symptoms that can be seen by others. If you could share one thing with the public about living with a chronic illness what would you want them to know?
To the teachers who think we are fake being sick, we are not faking.
For more information on IBD you can visit:
Centers For Disease Control and Prevention
Where You Can Follow Collin:
With Love,
Amber


